Salzmann’s nodular degeneration is a rare non-inflammatory and slowly progressive condition that may develop secondary to chronic keratitis, trachoma, and particularly phlyctenulosis. It differs from familial dystrophies in that it is usually unilateral and not genetically determined.
The condition is characterized by the appearance of elevated, whitish/blue, subepithelial nodules, and it can appear at any time in life. The epithelium is thinned and irregular, and the Bowman’s layer is usually replaced by scar tissue.
Frequently, the nodules cause no irritation but merely affect vision. However, in some cases, the symptoms may be severe, including sudden attacks of redness, irritation, and photophobia. In addition, fresh nodules may persistently appear over a period that can last for years.
Case Details
A 55-year-old male who referred to our clinic for correction of his unilateral irregular astigmatism secondary to Salzmann’s nodular degeneration. He reported symptoms of diplopia, ghosting, and starbursts. Entering visual acuities were right eye 20/400 without correction and left eye 20/20 with his habitual toric soft lens.
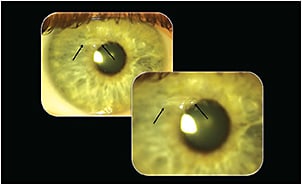
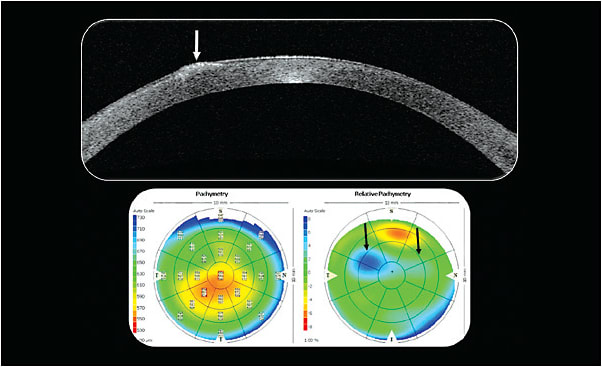
Slit lamp examination of the right eye showed an elevated, atypically long, 5.0mm lesion in the midperipheral cornea at 10 o’clock and a second, faint nodular scar at 2 o’clock (Figure 1). The left eye was completely free of any scaring or visible nodules. Simulated keratometric readings were 43.00 @ 008/45.50 @ 098 OD and 43.87 @ 005/47.00 @ 095 OS (Figure 2). Corneal thickness was measured with the Zeiss Visante (Carl Zeiss Meditec) and revealed a localized thickening (best seen in the relative pachymetry map) in the superior midperiphery of the right cornea and a normal thickness profile of the left eye (Figure 3).

We determined that the patient’s therapeutic and visual needs might be best served with a scleral lens for his right eye. The patient was subsequently fitted with a 14.8mm scleral lens. The lens diameter was selected based on the patient’s smaller-than-normal horizontal visible iris diameter (11.4mm), and his required sagittal height was well within normal sag limits. The final lens parameters were sagittal height of 3,600 microns, 7.85mm base curve, –1.75D power, and 14.8mm diameter (Figure 4). Visual acuity with his scleral lens was 20/25, and the patient was able to comfortably wear the lens for 16 hours a day.
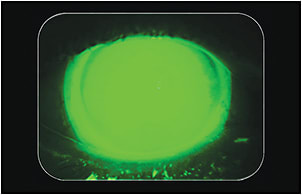
Elevated Fitting
The corneal vaulting properties of scleral lenses make them the ideal modality for eyes in which elevated lesions or nodules might be present. CLS
Patrick Caroline is an associate professor of optometry at Pacific University.
Mark André is an associate professor of optometry at Pacific University. He is also a consultant to CooperVision




